Welcome! First blog post – Health updates & Call to Action
Hi all,
Jenna has been in critical condition needing a double lung transplant since February 21st this year.
We are happy to share that despite many scary moments, long, painful battles, and a massive surgery, she has finally received her life-saving lungs!
Jenna’s new lungs birthday is March 19th – in honor of this huge milestone, it would be amazing to show Jenna love by donating $19 for the 19th to COTA for Jenna’s Lungs. Please consider if you are able, as the long and expensive road to recovery begins now. COTA.org/COTAforJennasLungs
We will be posting here for updates related to healing milestones and COTA for Jenna’s Lungs fundraising events.
Jenna’s family has been keeping track of her hospital course during her NYC admission – we are sharing that journey today.
Thank you all so much for your continued support!!
Love,
Jenna & family
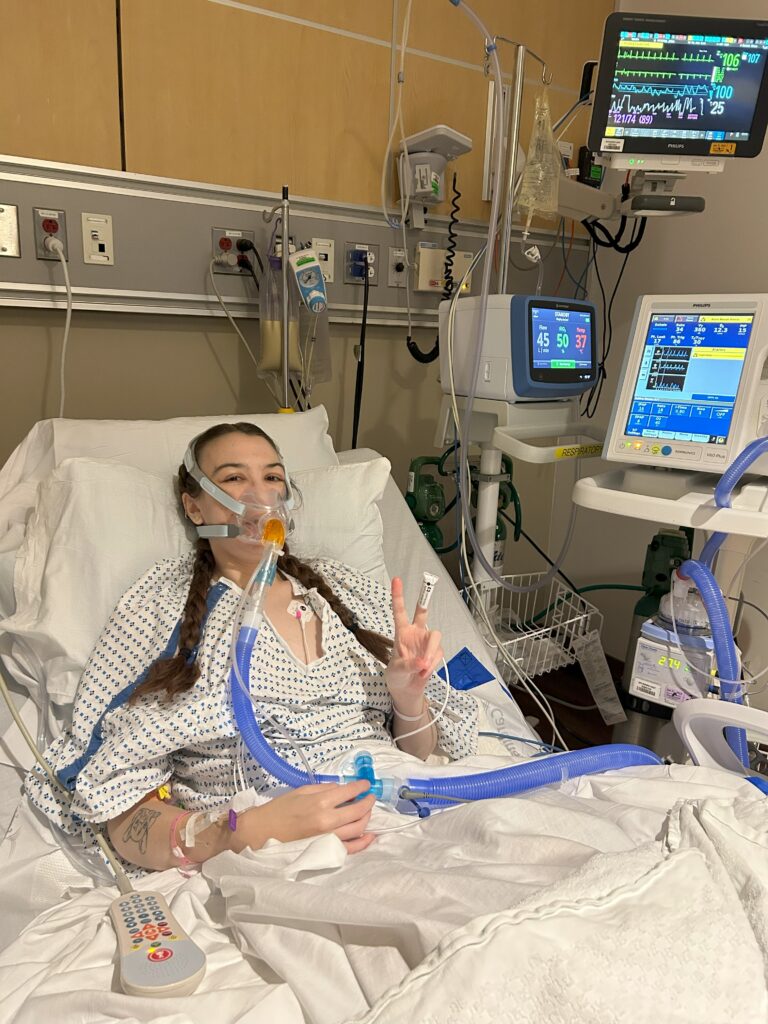
Jenna’s Hospital Course
2/21/24 – Jenna was admitted to Highland Hospital ICU in Rochester, NY when she wasn’t able to breathe at home. The doctors found her carbon dioxide levels to be in the 100s, way over normal range. She went on BiPAP – a positive pressure machine and mask over nose and mouth that pressure forces oxygen in and CO2 out. Her lung function had decompensated so much that she needed to be airlifted to NY Presbyterian, her designated lung transplant hospital in NYC in hopes of expediting work up and getting new lungs ASAP.
2/24/24 – On Saturday morning, Jenna took a medical plane to NYC, where she continued BiPAP in the ICU. She spent a few days getting tons of tests done and she doesn’t remember very much because the high CO2 levels impaired her consciousness. She had a midline placed for PN (intravenous food) and on tube feeds through her gastric tube to increase her weight as much as possible.
She was seen by many health care providers including ICU doctors, residents, physicians, and nurses, the transplant team, respiratory therapists, social workers, physical therapists, nutrition doctors, pulmonologists, infectious disease physicians, general medicine teams, and more. Throughout the week Jenna did trials of high flow oxygen instead of BiPAP.
2/27/24 – Jenna was stable enough to be transferred out of the ICU to a step down unit and started to eat some food. The BiPAP was only being used at night while high flow oxygen was being adjusted during the day. During physical therapy, Jenna started walking more and more each day with the help of 2 incredible people, Pete (physical therapist) and Craig (respiratory therapist) who brought humor and friendly demeanor every day. The transplant team was meeting with Jenna every day to take steps to get Jenna listed for lungs.
3/1/24 – Jenna approved for transplant! Now a waiting game with insurance to get listed. After a few days, Jenna was officially listed and the calls became coming in.
During the waiting game, Jenna had ups and downs. There were new pains and infections and her medications were changed many times. There were calls for lungs which Jenna accepted but ended up not being viable for Jenna at the last minute.
3/17/24 – Jenna decompensated and became unconscious. The code response team came and brought her to the ICU where she was intubated (tube down her throat with a machine breathing for her) and sedated. They found that her blood CO2 levels had spiked again. To help remove the CO2, she was placed on a machine called ECMO (extracorporeal membrane oxygenation) – a form of life support outside of her body that works as her lungs. Large central IV lines were placed in her legs and neck for her blood to come out of her body, be filtered by ECMO, and returned to her body. At this point, Jenna had 2 central lines in her neck, 2 IVs in her arms, an IV in her ankle, and a line in her port.
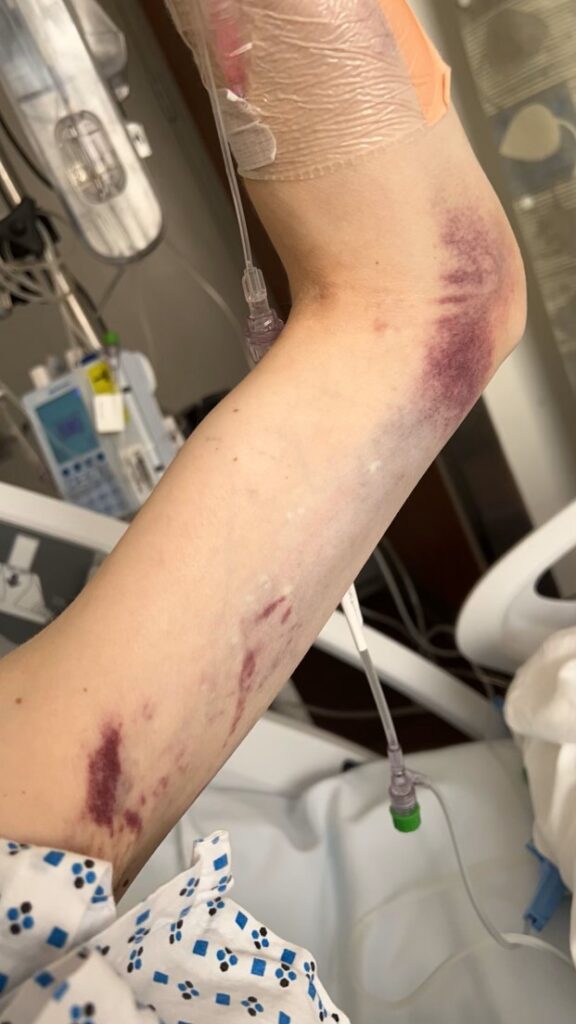
Within a couple days, Jenna had somewhat recovered, was extubated (tube in throat taken out) and was on BiPAP again. She developed a blood clot in her leg and had a procedure to get a filter placed in her vein so the clot doesn’t travel to her lungs. Despite becoming so sick, Craig and Pete got Jenna back on the treadmill and started walking again with the help of other team members, even with all of these lines and machines in place – amazing people! She received blood transfusions to keep her hemoglobin in a safe range.
Jenna was now top of the transplant list and considered super high priority. In total now she had received 4 calls for lungs that had not worked out, but that was about to change.
3/19/24 – While sitting in a chair after PT, Jenna received a call for the 5th set of lungs. These were the ones! She was called into surgery 2 hours later and underwent the major surgery to take out her old lungs and replace with new.
3/22/24 – After 3 days of being sedated in the CT (cardiothoracic) ICU post-surgery, Jenna woke up with new lungs in place! She remained intubated for the next 2 days, but was able to come off of ECMO. There were 4 tubes in her chest for drainage and had 72 staples in her chest to keep her chest wound closed. The incision is entirely across her chest from armpit to armpit.
3/24/24 – Jenna takes her first breath with her new lungs! Immediately she was on a very low amount of regular oxygen (big improvement from high flow prior to transplant), and within a couple days she was completely off oxygen and breathing on her own. The following days she was transferred down to the step down unit. She had swallow studies to make sure it was safe to start eating again, and had her chest tubes removed one at a time. A week later, she became a regular floor patient with no vitals or breathing help needed. She was off PN, didn’t need tube feeds, and was eating meals for her calories. She was on a pain medication pump for the pain after surgery, but that amount decreased over time.
4/5/24 – Jenna continued PT every day and finally had her 4th chest tube removed. She still did not need any nutrition support and was eating meals. She was having weekly clean outs of her lungs to get rid of any residual mucus and infection from the surgery, and feeling better after each one. She had to be on antibiotics for a bit longer until she was ready for discharge.
4/12/24 – The pharmacist came to do discharge counseling – Jenna has over 2 dozen post-transplant medications she will go home on. One of the anti-rejection medications (tacrolimus) requires close drug level monitoring and adjustments were made.
4/14/24 – Jenna had a complication prior to discharge. She was sick to her stomach, unable to eat, and was having severe arm tremors and seizures. These can be side effects of tacrolimus. A neurologist performed an EEG and ordered an MRI – they ended up looking good and the anti-rejection meds were adjusted.
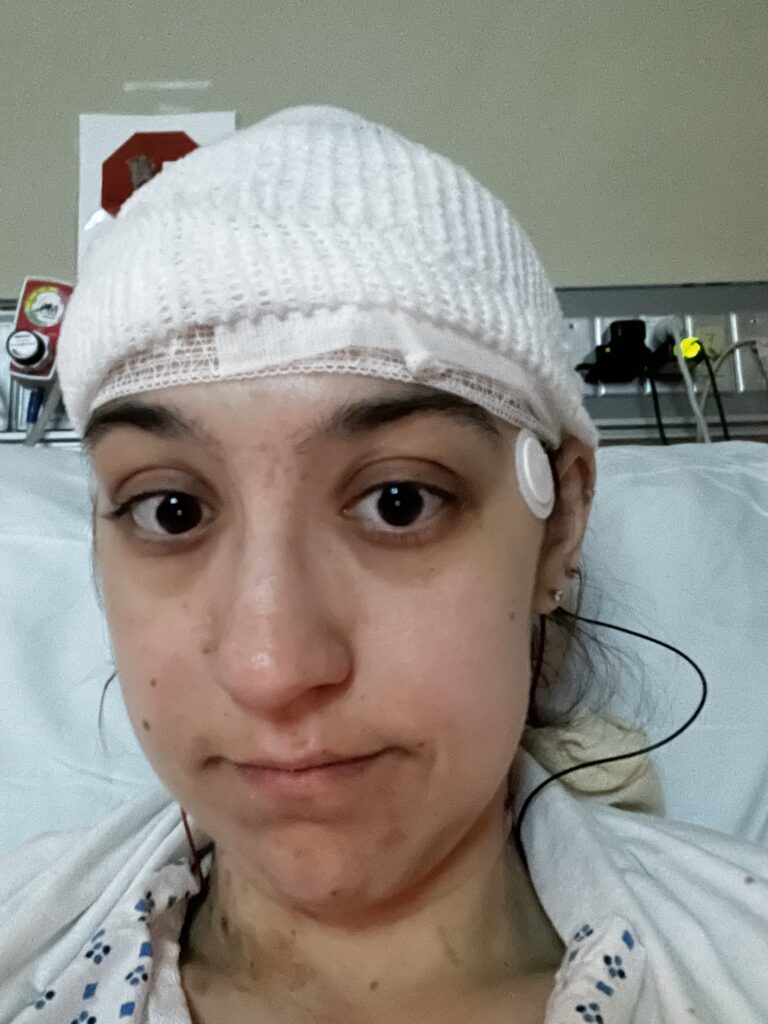
4/19/24 – Jenna thought she would be getting discharged, but instead woke up with severe stomach pain. The surgery team thought it might be her gallbladder, pancreas, or an ileus (inability of the intestine to contract normally and move waste out of the body). She went through episodes of acute pain, scans, and an endoscopy. After a few days, her gut slowly improved.
4/25/24 – DISCHARGE DAY! Jenna finally leaves the hospital. She has weekly follow ups for labs, lung tests, imaging, and medicine adjustments, and will get her staples out soon. Her and her family are staying at a hotel with a kitchen area a short drive away that allows pets so she will have Bailey by her side.
Stay tuned for future updates on Jenna’s road to recovery.
The Children’s Organ Transplant Association (COTA) helps children and young adults who need a life-saving transplant by providing fundraising assistance and family support. COTA is the nation’s only fundraising organization solely dedicated to raising life-saving dollars in honor of transplant-needy children and young adults. 100% of each contribution made to COTA in honor of our patients helps meet transplant-related expenses. COTA’s services are free to our families, and gifts to COTA are tax deductible to the fullest extent of the law.
