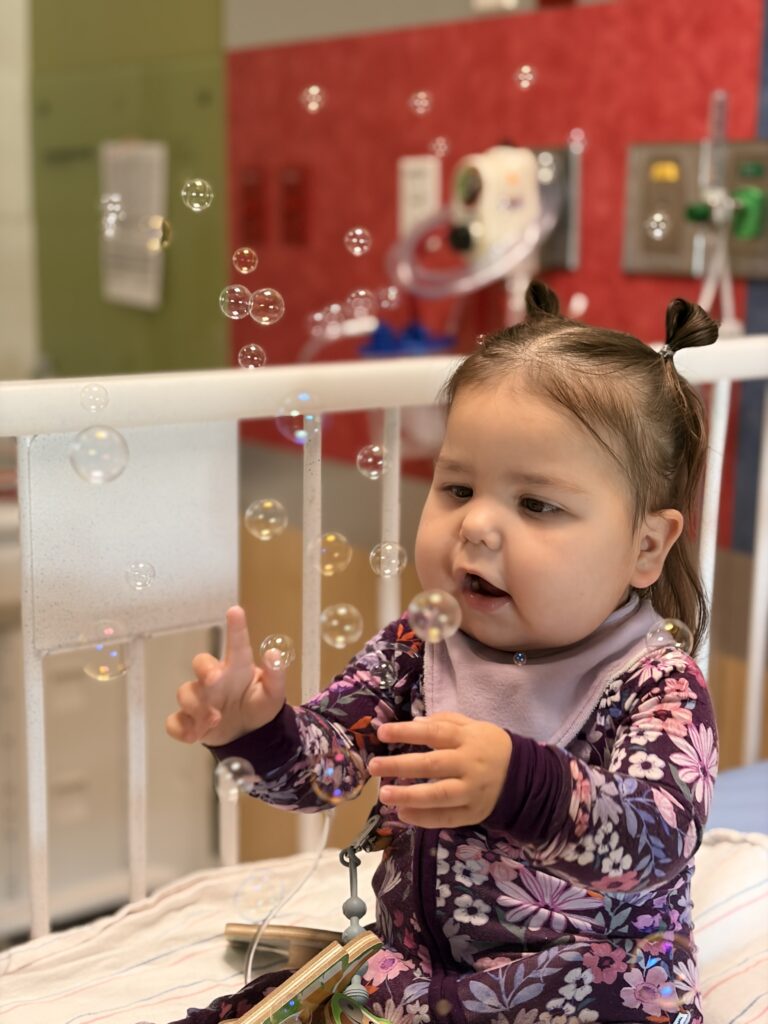
Today marks day 30 of our stay at Phoenix Children’s Hospital. We were admitted on January 5th for what we hoped would be a straightforward, planned admission. The goal was simple: Rylee needed an ostomy reversal before she could be officially listed for a kidney transplant.
Because of Rylee’s unique anatomy and her dependence on dialysis, her surgical plan was more complex than most. Along with the ostomy reversal, surgeons repaired a section of duplicated colon and placed a hemodialysis (HD) catheter. The plan was for her to transition to HD for four to eight weeks, then return to peritoneal dialysis (PD) once everything healed.
But Rylee had other plans.
About a week into our stay, things began to change quickly. Her oxygen levels started dropping, her heart rate climbed, and she developed persistent fevers. On January 15th, the nurses on the 8th floor called a rapid response. In that moment, her room filled with doctors as they assessed whether she needed to be transferred to the PICU.
Before making that decision, they sent her to radiology for a dye study and CT scan to check for a possible surgical leak. If one was found, the plan was for her to go straight to the PICU and then back to surgery.
The imaging confirmed our worst fear. Rylee had developed a small hole in her bowel, allowing stool to leak into her abdomen and spread infection. She was taken to surgery that same day.
Fortunately, the surgeons believed the hole would heal on its own. Instead of revising the stitches and risking further irritation, they created an ileostomy to reroute stool and give the new connection time to heal. They also placed two drains to remove infected fluid and stool and used a wound vac after reopening her previous ostomy incision.
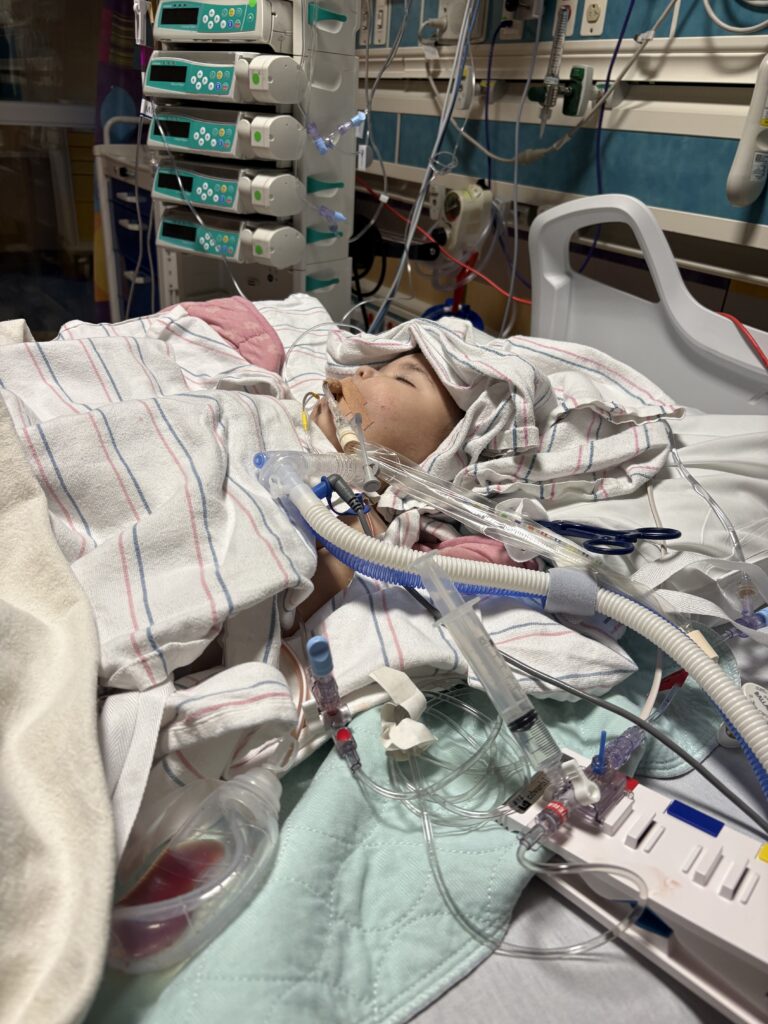
Rylee came out of surgery intubated and heavily sedated.
What followed has been a whirlwind of ups and downs. There was a successful extubation, followed by an emergency re-intubation. She has had more ultrasounds, CT scans, and blood transfusions than we can count. She’s gone to interventional radiology twice to drain additional fluid from her abdomen and back to the operating room to remove her infected PD catheter.
Through it all, Rylee has handled everything with incredible strength—helped along by sedation and pain medication, of course.
Today, we finally see some light. Rylee is extubated and appears to be feeling better. We are slowly weaning her off pain and sedation medications and continuing to adjust treatments to fight the infection. While in the PICU, she has been on continuous hemodialysis (CKRT), which allows fluid to be removed gently throughout the day while she receives nutrition through TPN.
For now, our days are filled with careful monitoring, medication weans, and oxygen support. We are hopeful that in the coming days her final drain can be removed and that these lingering fevers will finally subside.
This journey has been exhausting, terrifying, and overwhelming—but we cannot end this update without saying thank you. The love, prayers, messages, meals, and support from our friends and family have carried us through some of the hardest days. We are endlessly grateful, and we continue to hope and fight alongside our girl, one day at a time.